When we talk about blood pressure, we’re really discussing the pressure your blood exerts against your artery walls as it circulates. It’s a key health measure that shouldn’t be overlooked.
The American Heart Association (AHA) has put together an insightful blood pressure chart, drawing on numerous studies, both clinical and non-clinical. One standout reference is the 2018 study by Muntner et al., published in the Journal of Hypertension, emphasizing the need to consider variations in blood pressure readings, whether they’re taken at home or while on the move.
Grasping what your blood pressure numbers mean is vital. High or low blood pressure can be a stealthy health threat, often not showing symptoms but carrying significant risks.
To make sense of your readings, it’s important to familiarize yourself with the different levels of blood pressure:
- Low
- Normal
- Elevated
- High
- Hypertensive crisis
In many cases, especially in the initial stages, lifestyle adjustments rather than medication can effectively manage your blood pressure.
Blood pressure is typically measured using a device called a sphygmomanometer. This apparatus includes an inflatable cuff, which is wrapped around your arm and inflated to temporarily halt blood flow. As the cuff deflates, the device records the force exerted on your artery walls, yielding two numbers: systolic (the higher number indicating maximum pressure) and diastolic (the lower number indicating minimum pressure).
Exploring how we measure this crucial health indicator, devices like the Oxiline Pressure X Pro and CheckMe BP2 are notable. These modern tools are becoming increasingly popular for their accuracy and ease of use.
The significance of monitoring blood pressure is widely acknowledged. So much so, that many health enthusiasts and professionals recommend having a downloadable or printable version of the blood pressure chart. For your convenience, you can find such a chart at the end of this article.
What Exactly Is a Blood Pressure Chart?
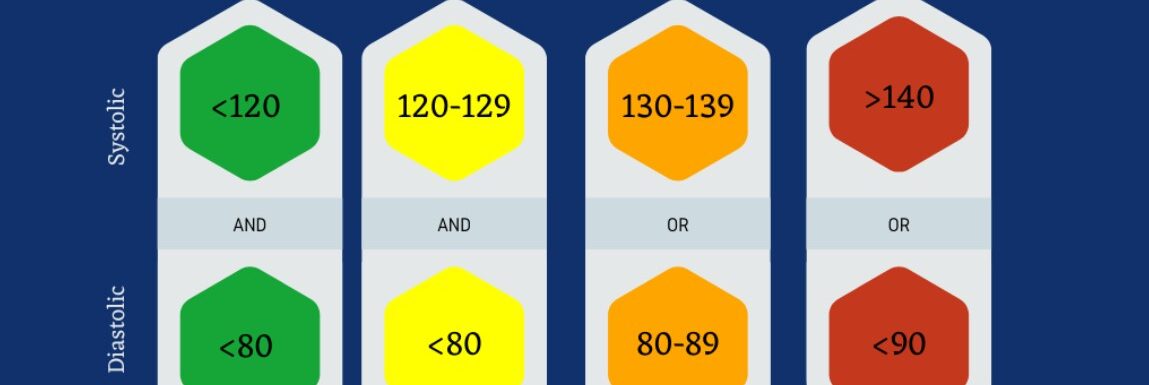
Have you ever wondered about the significance of a blood pressure chart? This tool is crucial in interpreting your cardiovascular health from the blood pressure readings you receive. It’s designed to categorize blood pressure into different ranges like low, normal, or high. Here’s an overview based on the American Heart Association’s latest guidelines:
- NORMAL BP: Systolic less than 120 mm Hg and Diastolic less than 80 mm Hg
- PRE-HYPERTENSION (Elevated Blood Pressure): Systolic between 120-129 mm Hg and Diastolic less than 80 mm Hg
- HIGH BP (Hypertension STAGE 1): Systolic between 130-139 mm Hg or Diastolic between 80-89 mm Hg
- HIGH BP (Hypertension STAGE 2): Systolic between 140-180 mm Hg or Diastolic between 90-120 mm Hg
- VERY HIGH BP (Hypertensive Crisis): Systolic higher than 180 mm Hg and/or Diastolic higher than 120 mm Hg
This chart isn’t just a set of numbers; it’s a vital tool for discussing health concerns with doctors and understanding treatment options, playing a significant role in enhancing heart health awareness and management.
Interestingly, low blood pressure, which can sometimes be an emergency situation, isn’t mentioned in the chart. It’s less common than hypertension, but the body typically provides alerts before it becomes a critical issue.
A notable update in the American Heart Association’s guidelines is the redefinition of high blood pressure. The threshold has been lowered from the previous benchmark of 140/90 mm Hg to 130/80 mm Hg. This change is based on clinical observations that symptoms of high blood pressure begin to manifest at the lower threshold.
Dr. Paul K. Whelton, the principal author behind these guidelines, highlights the risks associated with blood pressure readings in the range of 130-139/80-89 mm Hg. He points out that these levels double the risk of cardiovascular complications compared to individuals with normal blood pressure, emphasizing the need for increased vigilance and potentially non-pharmacological measures for managing blood pressure.
However, it’s important to note that these standards are not universal. Normal blood pressure readings are influenced by a variety of factors, including lifestyle, dietary habits, climate, and regional differences.
Understanding a blood pressure chart is crucial. The numbers you see could be the difference between a healthy life and a life-threatening condition. Knowing what each number represents and how it impacts your health is key to maintaining a healthy heart.
How to Read a Blood Pressure Chart?
When deciphering a blood pressure chart, it’s essential to focus on two crucial numbers that your blood pressure monitor displays. These figures, typically separated by a slash (for example, 120/80 mmHg), represent distinct aspects of how your heart functions.
The initial number is your systolic blood pressure, while the subsequent number denotes diastolic blood pressure. Comprehending these figures is key, as they provide significant insights into the state of your heart health, aiding in the early identification and handling of potential cardiovascular problems.
Let’s explore further the nuances of systolic and diastolic readings and their respective differences.
What Is the Difference Between Systolic and Diastolic Blood Pressure?
The primary distinction between systolic and diastolic blood pressure lies in what they measure regarding heart activity.
Systolic pressure, the upper number, gauges the pressure in your arteries during the moments your heart contracts and pumps blood. A normal systolic pressure is generally below 120 mmHg. Elevated systolic readings can suggest that your heart is exerting extra effort.
Conversely, diastolic pressure, the lower number, assesses the pressure in your arteries when your heart is in a state of rest between beats. A typical diastolic reading falls below 80 mmHg, indicating that your arteries are adequately relaxing.
According to a study by Tulane University researchers on “High Blood Pressure and Cardiovascular Disease,” abnormal values in either systolic or diastolic pressure can be indicative of health issues. It is crucial to recognize the importance of both systolic and diastolic measurements in providing a complete picture of heart health.
What Is the Meaning of mmHg in Blood Pressure Readings?
MmHg, short for millimeters of mercury, is the conventional unit used in blood pressure measurements. This unit’s prevalence dates back to the use of mercury sphygmomanometers in clinical settings, which established mmHg as the standard.
In mmHg, the blood pressure’s ability to push a mercury column to a certain height in a manometer or sphygmomanometer is measured. When blood pressure is recorded, it involves two levels: systolic (pressure during heartbeat) and diastolic (pressure between heartbeats). These are typically noted as one number over another, such as 120/80 mmHg, with both values expressed in millimeters of mercury.
This standardized metric is pivotal for health professionals to accurately assess and track blood pressure, aiding in the diagnosis and management of heart-related conditions.
Is kPa the Same as mmHg When Measuring Blood Pressure?
While kPa (kilopascals) and mmHg (millimeters of mercury) are both pressure units, they are not identical.
mmHg has been the traditional unit for blood pressure measurements in medical settings, primarily because of its historical association with mercury sphygmomanometers.
Gianfranco Parati and colleagues in their 2004 paper “Blood pressure measurement in research and in clinical practice: recent evidence” discuss the relevance of kPa in blood pressure measurement. To convert these units, understand that 1 mmHg is roughly equivalent to 0.133 kPa.
Therefore, a blood pressure reading of 120/80 mmHg would translate to approximately 15.99/10.66 kPa. However, it’s essential to recognize that clinical blood pressure measurements are generally not conducted in kPa, with mmHg being the universally accepted standard.
What are The Blood Pressure Stages/Ranges?
The American Heart Association categorizes blood pressure into five distinct levels to aid individuals and healthcare providers in evaluating cardiovascular health. These ranges include Normal, Elevated, High Blood Pressure Stage 1, High Blood Pressure Stage 2, and Hypertensive Crisis. Apart from these standard classifications, blood pressure is further differentiated into hypotension and severe categories for more detailed clinical assessment. Each of these classifications carries specific implications for heart health, which we will discuss in detail.
Very Low Blood Pressure (Severe Hypotension)
Severe Hypotension, or Very Low Blood Pressure, is a condition where blood pressure levels significantly fall below the normal range, potentially impairing blood flow to essential organs. This condition is a cardiac emergency, often defined by a blood pressure reading lower than 80/50 mmHg. Key aspects of severe hypotension include:
- Causes: Factors like dehydration, severe blood loss, heart diseases, endocrine disorders, sepsis, and certain medications can lead to severe hypotension.
- Symptoms: Symptoms often include dizziness, fainting, fatigue, nausea, blurred vision, and concentration difficulties.
- Dangers: It’s a life-threatening condition due to the risk of inadequate blood flow to crucial organs. Immediate medical attention is required.
- Treatment: Depending on the cause, treatments may involve medications, dietary changes, and addressing underlying health issues.
- Prevention and Management: Regular blood pressure monitoring, maintaining hydration, a balanced diet, and managing underlying health conditions can help prevent or manage severe hypotension.
Low Blood Pressure (Hypotension)
Hypotension, or Low Blood Pressure, is when blood pressure levels are below the normal range but not as severe as severe hypotension. This condition is not typically highlighted in AHA guidelines, as it’s usually benign unless causing symptoms. Hypotension is often considered when readings are below 90/60 mmHg but above 80/50 mmHg. Key facts about hypotension include:
- Causes: It can stem from dehydration, heart or endocrine problems, severe infections, significant blood loss, nutritional deficiencies, and certain medications.
- Symptoms: Symptoms may include dizziness, lightheadedness, fainting, blurred vision, fatigue, nausea, and difficulty concentrating.
- Dangers: If not addressed, hypotension can lead to inadequate blood flow to organs and the brain, which can be life-threatening.
- Treatment: Treatment varies based on the cause and may include medication, dietary supplements, and lifestyle changes.
- Prevention and Management: Effective management involves adequate fluid intake, small frequent meals, avoiding alcohol, careful posture changes, and managing underlying conditions.
Normal Blood Pressure
Normal Blood Pressure is when readings are within a standard range, ensuring adequate blood flow to vital organs. According to sources like Harvard Health Publications and the AHA, a normal reading is below 120/80 mmHg. Maintaining normal blood pressure is essential for cardiovascular health, reducing strain on the heart and arteries. Important considerations for normal blood pressure are:
- Maintenance: A heart-healthy lifestyle, including a balanced diet and regular exercise, is key to maintaining normal levels.
- Monitoring: Regular checks help detect any early deviations from the normal range.
- Medical Guidance: Regular medical check-ups are advisable, especially if there are known cardiovascular risk factors.
Elevated Blood Pressure (Prehypertension)
Prehypertension, or Elevated Blood Pressure, is when levels are above normal but not high enough to be classified as hypertension. This stage, a precursor to hypertension, suggests a higher likelihood of developing high blood pressure without preventive measures. Prehypertension is usually defined by readings between 120/80 mmHg and 129/89 mmHg. Key points about prehypertension include:
- Causes: It can be caused by a family history of hypertension, a high-sodium diet, lack of physical activity, obesity, and excessive alcohol consumption.
- Symptoms: Prehypertension often shows no clear symptoms, making monitoring essential.
- Dangers: Without intervention, it can progress to hypertension, increasing risks of heart disease and stroke.
- Treatment: Lifestyle changes such as a healthier diet, regular exercise, reduced sodium intake, and limited alcohol consumption are often recommended.
- Prevention and Management: Managing prehypertension involves a healthy lifestyle, stress management, regular exercise, and blood pressure monitoring to prevent hypertension.
High Blood Pressure (Stage 1 Hypertension)
Stage 1 hypertension occurs when blood pressure consistently falls within the range of 130-139 mmHg systolic or 80-89 mmHg diastolic. Recognized by the AHA as an initial indicator of potential cardiovascular issues, individuals with such readings are advised to seek medical consultation. Here are some insights into stage 1 hypertension:
- Causes: Excessive salt consumption, obesity, genetic factors, aging, and physical inactivity are common causes. Stress, kidney diseases, and certain medications are also contributing factors.
- Symptoms: This stage often lacks noticeable symptoms. However, some individuals might experience headaches, shortness of breath, or nosebleeds, although these are not definitive signs.
- Dangers: Early-stage hypertension heightens the risk of heart conditions, strokes, and kidney issues. Without proper management, it can escalate to more severe hypertension stages, but it isn’t considered an immediate medical emergency.
- Treatment: Lifestyle modifications, including a balanced diet and regular physical activity, are usually recommended. Depending on risk factors, blood pressure medications may be prescribed.
- Prevention and Management: Reducing salt intake, maintaining a healthy weight, engaging in regular exercise, moderating alcohol consumption, and managing stress effectively are crucial. Regular medical check-ups for blood pressure monitoring are also important.
High Blood Pressure (Stage 2 Hypertension)
Stage 2 hypertension represents a more critical form of high blood pressure, typically defined by readings of 140/90 mmHg or higher, but below 180/120 mmHg. Immediate medical intervention is necessary in this stage due to its severity. Key details about stage 2 hypertension include:
- Causes: Similar to stage 1, common causes are high salt intake, obesity, genetic predisposition, older age, and inactive lifestyles. Chronic conditions like kidney disease and hormonal imbalances, along with certain medications, can elevate blood pressure to this level.
- Symptoms: Many may not experience symptoms; however, possible signs include headaches, vision disturbances, chest discomfort, breathing difficulties, irregular heartbeats, and fatigue.
- Dangers: This advanced stage significantly increases the risk of heart-related events such as heart attacks, strokes, and heart failure. Prompt medical attention is advisable.
- Treatment: A more intensive treatment approach is often required, typically involving a combination of medications. Lifestyle changes continue to play an essential role.
- Prevention and Management: Prevention involves the same strategies as stage 1: reduced salt intake, weight control, regular exercise, alcohol moderation, and stress management. Regular blood pressure monitoring and adherence to medical advice are key for those diagnosed.
Hypertensive Crisis
In a hypertensive crisis, blood pressure soars to extremely high levels, exceeding 180/120 mmHg. Recognized by the AHA as a medical emergency, immediate action, such as calling 911, is crucial if symptoms are experienced. This crisis is divided into two categories: urgent and emergency. Essential information about a hypertensive crisis includes:
- Causes: Potential causes range from not taking prescribed blood pressure medications to kidney failure, heart attacks, strokes, adrenal gland issues, and the use of certain stimulants or over-the-counter medications and supplements.
- Symptoms: Symptoms vary but may encompass severe headaches, breathlessness, chest and back pain, numbness or weakness, speech difficulties, vision problems, and intense anxiety.
- Danger: A hypertensive crisis can precipitate life-threatening complications like pulmonary edema, brain swelling, or organ damage. If it involves organ damage, it’s classified as a hypertensive emergency.
- Treatment: Immediate hospitalization is typically necessary, often involving IV medications to rapidly lower blood pressure. Assessing for organ damage is vital, as it influences treatment strategies.
- Prevention and Management: Regular blood pressure monitoring, strict adherence to medication regimens, and swift medical response to symptoms or extremely high readings are critical. Avoiding triggers and risk factors is also key in managing and preventing hypertensive crises.
What Determines Normal Blood Pressure Across Ages and Genders?
Normal blood pressure can vary depending on age and gender, as reported in a 2001 study by the Journal of Hypertension. While the widely accepted standard for adults is 120/80 mmHg, it’s crucial to recognize that normal ranges can shift based on various factors, including age, gender, and even ethnicity and physiological conditions.
What Is a Normal Blood Pressure Range for Men?
For men, the standard for normal blood pressure is typically less than 120/80 mmHg, though this can differ based on age, lifestyle, and overall health. These are general guidelines, and individual variations are common. The normal ranges by age group for men are:
- Young Adults (20s-30s): Usually around 120/80 mmHg, considered the healthy standard.
- Middle-Aged Adults (40s-50s): Often slightly above 120/80 mmHg, reflecting a gradual increase with age.
- Senior Men (60s and Older): Commonly around 140/90 mmHg or higher, with a noticeable increase, particularly in systolic pressure.
What Is the Normal Blood Pressure Range for Women?
For women, a healthy blood pressure is ideally below 120/80mmHg, though this may fluctuate with age, health, and other factors. Dr. Jennifer Wong, M.D., has noted an increased risk of cardiovascular events in women with systolic pressures over 110 mmHg. Hormonal changes, especially during pregnancy and menopause, can affect these readings. Typical ranges for women are:
- Young Adults (20s-30s): Generally around 120/80 mmHg, often seen as the baseline.
- Middle-Aged Women (40s-50s): Usually around 120/80 mmHg, though hormonal shifts can cause variations.
- Senior Women (60s and Older): Often around 140/90 mmHg or higher, mirroring men in the same age group and indicating an increased risk of hypertension.
What Are Healthy Blood Pressure Levels for Children?
In children, normal blood pressure starts lower than in adults and gradually increases with age. It varies based on their age, sex, and height. It’s important to compare a child’s blood pressure with the standard percentiles for their age, gender, and height. Typical ranges for children are:
- Infants (0-12 months): 75/50 to 90/65 mmHg, as blood pressure develops.
- Toddlers (1-2 years): 80/50 to 100/70 mmHg, increasing with growth.
- Preschoolers (3-5 years): 85/55 to 105/75 mmHg, aligning closer to adult levels.
- School Age (6-9 years): 90/60 to 120/80 mmHg, influenced by physical and emotional factors.
- Pre-teens (10-12 years): 95/65 to 125/85 mmHg, affected by hormonal changes and growth.
- Teenagers (13-18 years): 100/70 to 130/90 mmHg, with a broader range due to lifestyle and hormonal factors.
What Should Young Adults Know About Blood Pressure?
Young adults, typically from late teens to early 30s, should aim for a blood pressure below 120/80 mmHg. This age group is expected to maintain the healthiest levels due to their evolutionary advantage, with cardiovascular risks increasing with age. Stress, diet, physical activity, and genetics are key influencing factors. The general blood pressure categories for young adults are:
- Normal Blood Pressure: Below 120/80 mmHg, indicating optimal heart health.
- Elevated Blood Pressure: Systolic 120-129 / Diastolic <80, a stage indicating potential hypertension risk.
- Hypertension Stage 1: Systolic 130-139 / Diastolic 80-89, where lifestyle changes or medication might be needed.
- Hypertension Stage 2: Systolic ≥140 / Diastolic ≥90, a more severe stage requiring medication and lifestyle adjustments.
What Is the Ideal Blood Pressure Range for the Elderly?
For individuals aged 65 and older, the ideal blood pressure is typically below 120/80 mmHg. However, due to age-related changes in the cardiovascular system, it’s not uncommon for blood pressure to be naturally higher in this age group. Readings up to 140/90 mmHg may still be acceptable for many elderly individuals, particularly if lowering them leads to side effects or if they have maintained these levels stably without complications. Nevertheless, personalized assessments and recommendations from healthcare professionals are crucial. The blood pressure categories for the elderly are:
- Normal Blood Pressure: Below 120/80 mmHg, with slightly higher readings sometimes acceptable.
- Elevated Blood Pressure: Systolic 120-129 / Diastolic <80, possibly an early indication of cardiovascular risk.
- Hypertension Stage 1: Systolic 130-139 / Diastolic 80-89, often requiring medical and lifestyle interventions.
- Hypertension Stage 2: Systolic ≥140 / Diastolic ≥90, indicating more severe hypertension, usually necessitating medication and lifestyle adjustments.
What Is a Healthy Blood Pressure Range During Pregnancy?
During pregnancy, a normal blood pressure reading is generally expected to be below 120/80 mmHg. However, physiological changes during pregnancy can lead to variations. Blood pressure may fluctuate throughout pregnancy, with certain elevations potentially indicating complications, thus necessitating regular monitoring. Any sudden increase or unusual symptoms should be promptly communicated to healthcare providers. The blood pressure ranges during different stages of pregnancy are:
- First Trimester: Typically below 120/80 mmHg, mirroring pre-pregnancy levels or slightly lower.
- Second Trimester: Often decreases, usually reaching its lowest point mid-pregnancy.
- Third Trimester: May return to first trimester levels or become slightly higher.
- Elevated Blood Pressure: Consistent readings of Systolic 120-129 / Diastolic <80 may suggest elevated blood pressure during pregnancy.
- Hypertension: Readings at or above 140/90 mmHg indicate hypertension.
- Preeclampsia: Characterized by high blood pressure and potential organ damage, often arising post-20 weeks of pregnancy.
How Does Average Blood Pressure Vary by Race/Ethnicity?
Average blood pressure can differ across racial and ethnic groups, as outlined by Dr. Anum Saeed and colleagues from the American College of Cardiology in their 2020 analysis. Genetics, socioeconomic status, diet, stress levels, and healthcare access contribute to these disparities. However, it’s important to avoid overgeneralizations, considering individual factors and lifestyles. A study by Rahul’s team from the Smith Center for Outcomes Research in Cardiology showed variations in average blood pressure among different ethnic groups in the U.S., influenced by genetic backgrounds. The average readings are:
- White Americans: Systolic 135.9 / Diastolic 72.8 mmHg
- Hispanic Americans: Systolic 139.6 / Diastolic 76.1 mmHg
- Black Americans: Systolic 141.0 / Diastolic 76.6 mmHg
- Asian Americans: Systolic 140.3 / Diastolic 76.3 mmHg
- Others: Systolic 134.7 / Diastolic 75.8 mmHg
What Is Normal Blood Pressure for Pets?
Normal blood pressure for pets varies between species, generally ranging from 110/60 to 170/100 mmHg. Blood pressure is a crucial health indicator in animals, much like in humans, reflecting their cardiovascular health. Different species and breeds have varying norms, and measuring blood pressure in pets requires specialized equipment and techniques. Typical blood pressure readings for common pets are:
- Dogs: 110-160/60-100 mmHg, with variations based on breed size.
- Cats: 120-170/55-100 mmHg, less frequently measured in diagnostic settings.
- Birds and Exotic Pets: Varies significantly, with specific reference values often challenging to establish due to limited research. Blood pressure measurement is less common than in dogs and cats.
Why Is Blood Pressure Monitoring Crucial?
Monitoring blood pressure is a key step in maintaining heart health. Its importance is multifaceted, as outlined in the following points:
- Early Detection: Regular monitoring can identify hypertension or other cardiovascular issues early, often before symptoms are noticeable. This early detection facilitates timely intervention, potentially reducing the risk of severe complications.
- Treatment Assessment: For those on antihypertensive medications, tracking blood pressure helps in evaluating the effectiveness of the treatment, allowing for necessary adjustments.
- Prevention of Serious Health Issues: Unchecked high blood pressure can lead to major health problems like heart attacks, strokes, and kidney diseases. Monitoring aids in circumventing these issues.
- Understanding Risk Factors: Consistent observation of blood pressure readings can illuminate the impact of lifestyle choices, such as diet, exercise, stress levels, and smoking habits.
- Managing Other Health Conditions: Conditions like diabetes, kidney diseases, and heart issues can influence blood pressure. Regular monitoring assists in holistic management of these health concerns.
- Avoiding Hypertensive Crisis: Extremely high blood pressure readings can precipitate a hypertensive crisis, necessitating emergency treatment. Regular checks help in preventing such emergencies.
- Overall Health Maintenance: Even for those without hypertension risks, periodic blood pressure checks offer insights into cardiovascular health, promoting a proactive health mindset.
- Motivating Lifestyle Changes: Recognizing trends in blood pressure can encourage beneficial lifestyle modifications, such as healthier eating, regular physical activity, and effective stress management.
How Can You Accurately Measure Blood Pressure at Home?
Measuring blood pressure at home involves a series of steps to ensure accuracy:
- Selecting a Monitor: Opt for a reliable home blood pressure monitor. Models like the Oxiline Pressure X Pro or CheckMe BP2 are often recommended for their precision.
- Proper Positioning: Sit in a comfortable chair at a table, ensuring your arm is at heart level. Your feet should be flat on the floor with your back supported.
- Cuff Placement: Fit the cuff snugly on your bare upper arm, making sure it’s neither too tight nor too loose.
- Preparation: Spend about 5 minutes relaxing before starting the measurement to guarantee accurate results.
- Taking the Measurement: Turn on the monitor to take the reading. To get the most precise reading, it’s advisable to take two or three readings, spaced a minute apart, and calculate the average of these.
Careful adherence to these steps can ensure your home blood pressure readings are as reliable as those taken by a healthcare professional.
Which Blood Pressure Monitors Are Most Reliable?
The most reliable blood pressure monitors for accurate at-home readings are produced by three brands: Oxiline, CheckMe, and QardioArm. Below is a comprehensive comparison of these products:
- Oxiline Pressure X Pro:
- Provides clear blood pressure range indications.
- Measures blood pressure, heart rate, and pulse accurately.
- Includes a built-in schedule chart for planning future readings.
- CheckMe BP2A:
- Features an innovative design for easy handling and portability.
- Offers Bluetooth connectivity for mobile data display.
- One-button start for BP and ECG information.
- QardioArm:
- Capable of detecting irregular heartbeats and delivering precise blood pressure readings.
- Offers output via a mobile app in visual graphs and charts.
- Compatible with various handheld devices.
Oxiline stands out in the market, particularly the Oxiline Pressure X Pro, known for its innovation and high praise in reviews, including recommendations from some clinicians. CheckMe follows closely with its BP2 and BP2A models, preferred for comprehensive cardiac health monitoring due to their smart features and smartphone integration.
How to Lower Blood Pressure Naturally?
Lowering blood pressure naturally involves various strategies, which, when followed diligently, can be effective:
- Dietary Changes: Incorporate a low-sodium diet, consume potassium-rich foods like bananas, increase fiber with whole grains, fruits, and vegetables, and consider the DASH diet that focuses on fruits, vegetables, and low-fat dairy.
- Physical Activity: Regular exercise is key, with 150 minutes of moderate-intensity or 75 minutes of vigorous-intensity aerobic activity weekly, plus strength training at least twice a week.
- Lifestyle Choices: Limit alcohol and caffeine intake, manage stress through relaxation techniques and adequate sleep, maintain a healthy weight, and eliminate smoking.
- Hydration: Drink plenty of water to stay hydrated throughout the day.
- Natural Supplements: Consider supplements like Omega-3 fatty acids, garlic, and flaxseed, but always consult a healthcare professional beforehand.
For those pursuing natural heart care, understanding baseline blood pressure figures is crucial.
Where Can You Find a Printable Blood Pressure Chart?
In our digital era, physical health management tools like a printable blood pressure chart can be very useful.
These charts allow for easy tracking and visualization of blood pressure readings over time, whether for personal use, sharing with healthcare providers, or assisting a loved one.
To download a printable blood pressure chart directly to your inbox, consider subscribing to relevant health newsletters. These charts can serve as a valuable tool in managing and understanding your blood pressure trends.